Providing professional care in fertility, gynaecology and minimally invasive surgery
Fibroids
Overview
Uterine Leiomyomata (singular, leiomyoma, also known as fibroids) are benign tumours arising from smooth muscle cells of the uterus. They contain normal tissues albeit in abnormal proportions. They are often surrounded by a thin layer of compressed collagen tissue and muscle fibres, referred to as a pseudocapsule.
Classification
Fibroids are usually described according to their locations within the uterus. The location of any particular fibroid can vary from time to time, according to fibroid growth, stage of menstrual cycle and the means used to assess it. Interestingly fibroids that lie in different positions in the uterus have a different genetic make-up, so they probably reflect subtly different diseases.
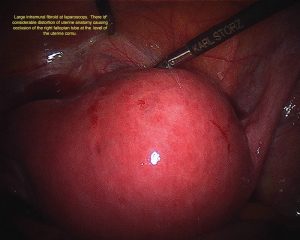
Intramural Fibroids
Intramural fibroids lie within the wall of the uterus. They may enlarge sufficiently to distort the outside of the uterus or the cavity of the uterus and may indeed extend from one side to the other.
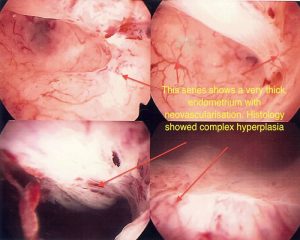
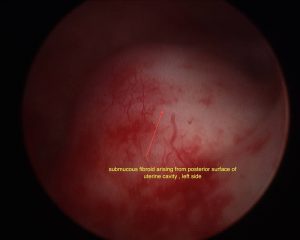
Sub mucosal Fibroids
Sub mucosal fibroids chiefly lie beneath the lining (endometrium) of the uterus. It is these that are chiefly responsible for disturbance in menstrual function, usually heavy periods. The extent of the protrusion into the endometrial cavity is described by the European Society of Hysteroscopy Classification system as follows:
- A type 0 fibroid is completely intra-cavity
- A type 1 fibroid has at least 50% of its volume in the cavity
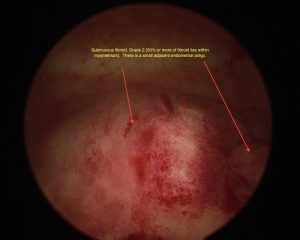
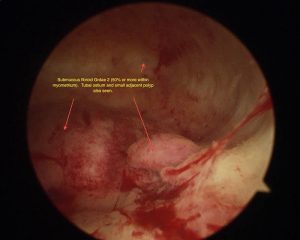
- A type 2 fibroid has at least 50% of its volume in the uterine wall
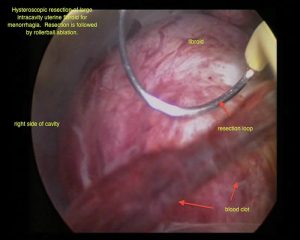
Type 0 and 1 can be removed by hysteroscopic resection, whereas those that lie within the muscle of the uterus can often only be removed in part by this method.
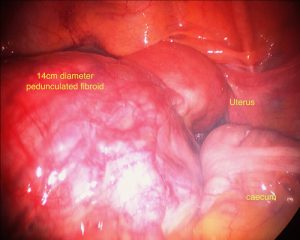
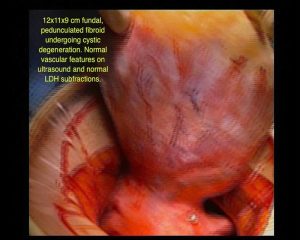
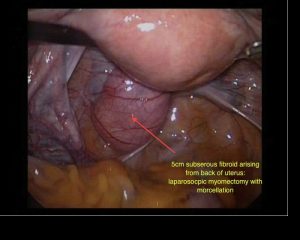
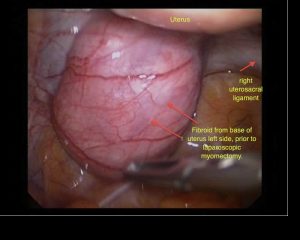
Sub serosal Fibroids
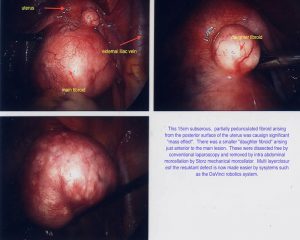
Sub serosal fibroids are those lying in the outer layers of the uterus. They may have a narrow base in which case they are described as pedunculated. Sometimes they can extend from the outer uterine surface to lie within the broad ligaments, which are the peritoneal coverings covering the fallopian tubes and blood vessels that enter the uterus. These can be difficult to remove.
Cervical Fibroids
Cervical fibroids are located in the cervix rather than the body of the uterus.
Fibroids and Fertility
Do all fibroids impact upon fertility?
The short answer is no. Fibroids are estimated to account for, or contribute to around 1-2% of infertility. Fibroids that distort the lining of the uterus (endometrium) affect fertility by means that are at present, incompletely understood. Possibilities include:
- The endometrial vascularity over the fibroid may be altered, reducing fertility and
- There may be differences in the biochemical milieu and contractility of the uterus at the site of the fibroid.
Importantly, the location of the fibroid and not it’s absolute size is the key factor in whether or not it may affect fertility. Even very small fibroids, when distorting the endometrial cavity, may impact on fertility whereas large fibroids on the outside of the uterus may not. The issue of fibroids within the uterine musculature (intramural) is more difficult. At present, it is thought that intramural fibroids, of 4cm or more do affect fertility, but removing these fibroids may not necessarily restore spontaneous fertility rates to normal. Note that this is different in the case of IVF.
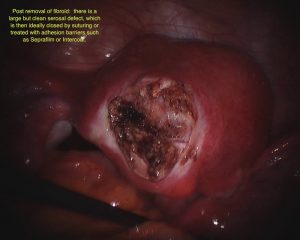
I strongly suspect that although removing these fibroids results in a fertility gain, some of that gain is negated with resultant adhesions. Thus the onus is on the gynecologist to remove the fibroid, returning the uterus in as perfect a fashion as possible, restoring myometrial continuity, with little chance of infection, hematoma or subsequent adhesion formation. This requires a meticulous surgical technique and I believe anti-adhesive measures to play a role. Please see Laparoscopic Removal of Fibroids for further discussion.
Do all fibroids interfere with a pregnancy?
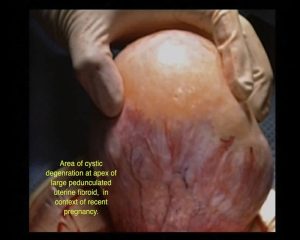
Once again, the answer is no. Everything depends on the site and size of the fibroid. Interestingly if in comparing groups of women with and without submucosal fibroids, once they are pregnant the miscarriage rate is similar.
Around 50 to 60% of fibroids increase in size during pregnancy. Most of this growth occurs during the first trimester, slowing in the second and third trimesters. Large fibroids greater than 5cm are more likely to grow where as smaller fibroids may remain stable. Size remains roughly stable after pregnancy, but about 10% will decrease in volume by around 10%. It is important to realise that both the uterus and the fibroids increase in size by processes of hyperplasia and hypertrophy i.e. more muscle cells and greater size in muscle cells. The tissue cannot completely disappear after pregnancy but may shrink somewhat. Many women with fibroids do not have any complications during pregnancy related to the fibroid. Complications may however occur, with pain being the most common. To summarise, the effects of fibroids on pregnancy may include:
- Miscarriage
- Premature labor and delivery
- Abnormal fetal position requiring operative delivery
- Placental abruption (the placenta peels away from the lining of the uterus)
- Abnormal fetal growth
- Morbidly adherent placenta (placenta unable to be expelled after the birth)
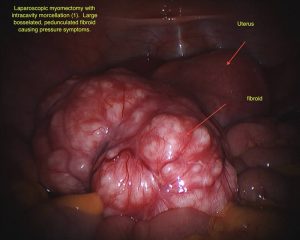
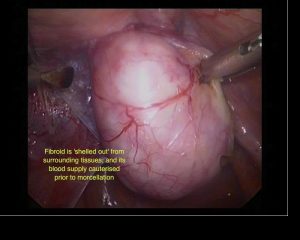
Laparoscopic Treatment Of Fibroids – (Laparoscopic Myomectomy)
Laparoscopic Myomectomy is a surgical procedure in which a fibre optic instrument is inserted through the abdominal wall in order to remove uterine leiomyomata (fibroids).
Reasons For Laparoscopic Myomectomy
There are many reasons for removing fibroids, which will vary from person to person in their type, size and significance. In the vast majority of cases where removal of fibroids is required, a laparoscopic route is appropriate. This can either be achieved by conventional “straight stick” laparoscopy or by Da Vinci (robotic) myomectomy. Data on post-operative recovery and effects of laparoscopic myomectomy versus open or laparotomy myomectomy, varies due to the extremely heterogeneous nature of the patients and surgeons skills in the studies. However, the benefits of laparoscopy are well proven with respect to decreased complication and improved recovery times. There are also undoubted cosmetic advantages to operating with small incisions.
It is usual for the laparoscopic myomectomies that I perform to be discharged on the same day.
Are all fibroids able to be removed laparoscopically
The short answer here is ‘no’ but in the vast majority of cases, this will be possible. It is not until the size of the fibroid approaches the height of the umbilicus (belly button) that serious issues may occur. However, with appropriate planning, pre-operative preparation and surgical skills, almost all problems can be avoided. Difficult procedures involve very large fibroids, patients of increased body mass index and cases where multiple fibroids co-exist. In these cases it is difficult, by any means, to preserve a sufficient amount of uterine muscle in order to affect a neat and sound repair of the uterus. Some fibroids regardless of size and according to location are easily removed. For example, fibroids at the front and centre of the uterus are generally easier to remove by any means. Difficult cases may be those where the fibroids extend into the coverings around the sides of the uterus (broad ligaments), especially if the fibroid has multiple parts and surrounds or pushes under the ureters.
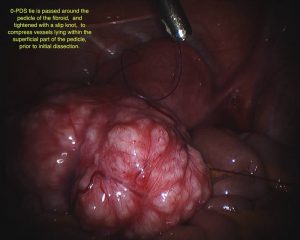
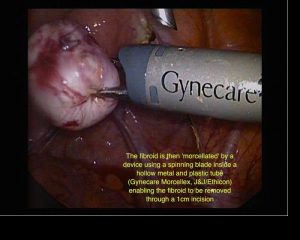
What we are able to do today is far in excess of that which was commonly done even two years ago. This has been made possible by improvements in sutures (specifically unidirectional barbed sutures), suturing technique, diathermy instruments, adhesion barriers, new haemostatic matrices, understanding of injectable haemostatic agents and morcellators. The latter are instruments that reduce fibroids to small strips so that they can be removed via small incisions.